Volume 19, Number 10—October 2013
CME ACTIVITY - Research
Cryptococcus gattii Infections in Multiple States Outside the US Pacific Northwest
Introduction

Medscape, LLC is pleased to provide online continuing medical education (CME) for this journal article, allowing clinicians the opportunity to earn CME credit.
This activity has been planned and implemented in accordance with the Essential Areas and policies of the Accreditation Council for Continuing Medical Education through the joint sponsorship of Medscape, LLC and Emerging Infectious Diseases. Medscape, LLC is accredited by the ACCME to provide continuing medical education for physicians.
Medscape, LLC designates this Journal-based CME activity for a maximum of 1 AMA PRA Category 1 Credit(s)TM. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
All other clinicians completing this activity will be issued a certificate of participation. To participate in this journal CME activity: (1) review the learning objectives and author disclosures; (2) study the education content; (3) take the post-test with a 70% minimum passing score and complete the evaluation at www.medscape.org/journal/eid; (4) view/print certificate.
Release date: September 19, 2013; Expiration date: September 19, 2014
Learning Objectives
Upon completion of this activity, participants will be able to:
• Distinguish characteristics of Cryptococcus gattii infection
• Analyze the clinical presentation of C. gattii infection in the United States
• Evaluate the management of C. gattii infection
• Distinguish outcomes of C. gattii infection.
CME Editor
Cathy Young, Copyeditor, Emerging Infectious Diseases. Disclosure: Claudia Chesley has disclosed no relevant financial relationships.
CME Author
Charles P. Vega, MD, Health Sciences Clinical Professor; Residency Director, Department of Family Medicine, University of California, Irvine. Disclosure: Charles P. Vega, MD, has disclosed no relevant financial relationships.
Authors
Disclosures: Julie R. Harris, PhD, MPH; Shawn R. Lockhart, PhD; Gail Sondermeyer, MPH; Duc J. Vugia, MD, MPH; Matthew B. Crist, MD, MPH; Melissa Tobin D’Angelo, MD; Brenda Sellers; Carlos Franco-Paredes, MD, MPH; Monear Makvandi, MPH; Chad Smelser, MD; John Greene, MD; Danielle Stanek, DVM; Kimberly Signs, DVM; Randall J. Nett, MD, MPH; Tom Chiller, MD, MPH; and Benjamin J. Park, MD, have disclosed no relevant financial relationships.
Abstract
Clonal VGII subtypes (outbreak strains) of Cryptococcus gattii have caused an outbreak in the US Pacific Northwest since 2004. Outbreak-associated infections occur equally in male and female patients (median age 56 years) and usually cause pulmonary disease in persons with underlying medical conditions. Since 2009, a total of 25 C. gattii infections, 23 (92%) caused by non–outbreak strain C. gattii, have been reported from 8 non–Pacific Northwest states. Sixteen (64%) patients were previously healthy, and 21 (84%) were male; median age was 43 years (range 15–83 years). Ten patients who provided information reported no past-year travel to areas where C. gattii is known to be endemic. Nineteen (76%) patients had central nervous system infections; 6 (24%) died. C. gattii infection in persons without exposure to known disease-endemic areas suggests possible endemicity in the United States outside the outbreak-affected region; these infections appear to differ in clinical and demographic characteristics from outbreak-associated C. gattii. Clinicians outside the outbreak-affected areas should be aware of locally acquired C. gattii infection and its varied signs and symptoms.
Cryptococcus gattii, a fungal pathogen found in the environment, is associated with soil and decaying organic debris. Infection in humans results from inhalation of spores from the environment and typically causes pneumonia or meningitis (1,2); the incubation period is thought to be 2–13 months, although it may be longer (3,4). Unlike the related species C. neoformans, which is distributed globally and is a common opportunistic infection in HIV-infected or severely immunocompromised persons, C. gattii typically affects patients without HIV infection (1,2,5–8), and its environmental distribution is thought to be more limited (9–11). C. gattii infection is typically considered more difficult to treat than C. neoformans infection and requires longer and more aggressive treatment (1,7,8,12,13).
Before 1999, clinical isolates of C. gattii were rare in North America; a small number of cases were reported, mostly in southern California and in Hawaii (9,10,14,15). However, since 2004, an outbreak of C. gattii cryptococcosis has been ongoing in British Columbia, Canada, and the US Pacific Northwest states of Washington and Oregon (2,5). Approximately 100 C. gattii cases have been reported from Washington and Oregon. The US Pacific Northwest outbreak is characterized by infection with 3 clonal C. gattii strains (VGIIa, VGIIb, and VGIIc), 2 of which are uncommon outside this region and 1 (VGIIc) that is unique to the region (16). Previously reported cases of C. gattii infection were in otherwise healthy patients who had severe central nervous system (CNS) disease (1). In contrast, most patients associated with the US Pacific Northwest outbreak have had respiratory symptoms and preexisting immunocompromising or other serious underlying medical conditions before becoming infected with C. gattii (2).
The outbreak in the US Pacific Northwest has increased interest in C. gattii among public health authorities and the US health community and resulted in efforts by the Centers for Disease Control and Prevention (CDC; Atlanta, GA, USA) to collect surveillance data on C. gattii infections from states outside that region. Whether these reported cases are an effect of the US Pacific Northwest outbreak on other areas of the United States and the implications for clinical care and broader surveillance have not been addressed. We summarize C. gattii cases reported to CDC from non–US Pacific Northwest states and discuss their implications.
A case was defined as a culture-confirmed C. gattii infection in a resident of the United States outside of Oregon or Washington who had no known recent travel history (within 1 year) to these states and had illness onset after January 1, 2009. Cases were reported to CDC by state health departments or physicians who were treating patients with suspected C. gattii infection (typically because the patient was not infected with HIV). Isolates were sent to CDC for confirmation; isolates were plated on differential canavanine-glycine-bromothymol blue medium (17), and molecular type and subtype were identified by using multilocus sequence typing at 7 loci (18). Neighbor-joining trees were developed by using the multilocus sequence typing results and MEGA 4.0 software (www.megasoftware.net). State and local health department staff and treating physicians completed standardized case report forms with demographic and clinical information on case-patients and submitted these reports to CDC. Sites of infection were determined as follows: for pulmonary, blood, cerebrospinal fluid (CSF), or tissue specimens, culture was considered evidence of infection at that body site. Histopathologic examination results demonstrating Cryptococcus yeasts in tissue also was considered evidence of infection at the tissue site. Cryptococcal antigen in the CSF was considered evidence of CNS infection; however, serum cryptococcal antigen in the absence of a bloodstream cryptococcal isolate was not considered evidence of a bloodstream infection.
Twenty-five cases for which descriptive data were available were identified in Alabama (1 case), California (13), Florida (1), Georgia (5), Hawaii (1), Michigan (1), Montana (1), and New Mexico (2). Some cases have been published as individual case reports (2,19–21). Twenty-one (84%) patients were male; median age was 43 years (range 15–83 years) (Table 1, Appendix). All patients had illness onset during January 2009–May 2012.
All patients except 1 were symptomatic. The single case in an asymptomatic patient was diagnosed by a chest radiograph during a post-trauma hospitalization; the radiograph showed upper lobe abnormalities. Four patients died before diagnosis; among the 21 patients surviving to diagnosis, the median time from symptom onset to diagnosis was 32 days (range 2–263 days). The most common symptoms were headache (67%), blurred vision (62%), and nausea (46%) (Table 1, Appendix). Leukocyte counts for 17 patients at diagnosis ranged from 6,400–20,700/mm3 (median 11,700); CD4 counts, available for 4 patients, ranged from 92 cells/mm3 to 838 cells/mm3 (median 595 cells/mm3). Twenty-three (92%) patients were hospitalized for a median of 23 days (range 1–88 days); 10 (48%) of 21 patients with data required admission to the intensive care unit. Results of lung imaging were abnormal for 19 (83%) of 23 patients with images; 14 (61%) had documented lung cryptococcomas. Results of head imaging were abnormal in 15 (75%) of 20 patients with images; 10 (50%) patients had documented brain cryptococcomas. Nineteen (76%) patients had culture, histopathologic, or serologic evidence of CNS infection, either alone or with pulmonary, blood, or tissue infections (Table 1, Appendix). Nine (36%) patients had culture or histopathologic evidence of pulmonary infection; 5 had isolated pulmonary infections. For 4 patients, C. gattii was isolated from blood samples.
Sixteen (64%) patients were otherwise healthy at diagnosis (Table 1, Appendix). Five (20%) patients had immunocompromising conditions (Table 1, Appendix): pulmonary sarcoidosis (CD4 count of 92 cells/mm3), diabetes and liver transplant, an unspecified immunocompromising condition, active lung cancer (patient receiving chemotherapy), and congenital hyper-IgE syndrome (Job syndrome). Four (16%) additional patients had nonimmunocompromising underlying disease at diagnosis. For the 12 patients with documented HIV test results, all results were negative.
Six patients (ages 18, 36, 39, 56, 68, and 82 years) died, all from their C. gattii infections (Table 2, Appendix). Three were previously healthy, 1 had multiple nonimmunocompromising underlying medical conditions, and 2 were immunocompromised. One of the 3 previously healthy patients (18-year-old woman) had a fulminant course of illness that led to death 2 weeks after onset. This patient sought treatment at a community hospital with headache, fever, and flat affect; she received ceftriaxone for a urinary tract infection and was hospitalized for suspected pseudoseizures. On day 4 of her hospitalization, she became lethargic and had a low-grade fever (100.8°F). A lumbar puncture (opening pressure >60 mm H2O) showed evidence of yeast; she was given liposomal amphotericin B and 5-flucytosine and was transferred to a referral hospital, where she received a lumbar puncture to drain CSF and endotracheal intubation for mechanical ventilation in the intensive care unit. Despite intensive supportive care, she died 2 days later of brain stem herniation caused by persistent elevated intracranial pressure (ICP).
In addition to this patient, 4 patients died before (or on the day of) their diagnoses, and 1 died 263 days after diagnosis (from shunt blockage). Three of the 4 who died before diagnosis had bloodstream infections. Three of the 4 female patients died; female sex (relative risk [RR] 5.3, 95% CI 1.6–17.3; p = 0.03) and having cryptococci isolated from blood (RR 5.3, 95% CI 1.6–17.3; p = 0.03) were significantly associated with increased risk for death. Death was not associated with other clinical or demographic variables.
Of the 21 patients surviving to diagnosis, treatment data were available for 19 (90%). All 17 who survived to diagnosis with bloodstream or CNS infections were initially given amphotericin B or liposomal amphotericin B; 16 also were given 5-flucytosine or fluconazole, and 1 was given amphotericin B alone. Of the 4 with isolated pulmonary infections who survived to diagnosis, 1 was given fluconazole alone, and 1 received amphotericin B and flucytosine; for 2, no treatment data were available.
Seven patients were given corticosteroids to treat their infection. One patient was given interferon. Twelve (57%) of 21 patients surviving to diagnosis had diagnostic or interventional surgeries, including 6 who needed a ventriculoperitoneal shunt or lumbar drain for refractory elevated ICP, 4 who needed brain or lung biopsies, 1 requiring placement of a chest tube for pleural effusion, and 1 requiring leg surgery at the infection site (21). Hydrocephalus developed in 4 (22%) of 18 patients with data, and cranial nerve palsies developed in 5 (38%) of 13 with data.
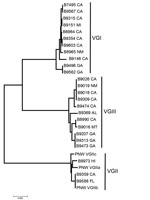
C. gattii isolates from patients were typed as VGI (11 [44%]), VGIII (11 [44%]), VGII (non–outbreak strain; 1 [4%]), and VGIIb (2 [8%]) (Table 3). Fifteen sequence types were represented among the 25 isolates, indicating a high degree of genetic diversity (Figure). One of the 2 VGIIb isolates was from an immunocompromised female patient from California with unknown travel history; the other was from an immunocompetent man from Florida with a leg infection and meningitis who reported no out-of-state travel for the past 20 years (21) (Table 1, Appendix; Table 3). Of the 13 California patients (reported from northern and southern California), 9 had unknown travel history, 2 had traveled to Mexico, and 2 had traveled to a central or eastern state in the year before their illnesses (Table 3). Ten patients (excluding the California patients) reported no exposure to known disease-endemic areas for at least the past year; 7 patients (1 from Alabama, 3 from Georgia, the Florida patient, the Montana patient, and 1 of the 2 New Mexico patients) reported no out-of-state travel for at least the past year (Table 3); 2 of these patients (New Mexico and Montana) were incarcerated, both for <1 year, in their home states before their illness onset. Eight had outdoor exposures involving construction or gardening during the year before their illness.
We describe severe C. gattii infections in the United States, many probably acquired in states outside the outbreak-affected Pacific Northwest. Most of these cases differed clinically and genetically from outbreak strains of C. gattii that are causing disease in the US Pacific Northwest, and they are unlikely to be associated with the outbreak. Ten patients with travel history had not traveled to areas where C. gattii is known to be endemic for at least 1 year before illness onset, suggesting that C. gattii may be endemic in some areas of the United States outside the Pacific Northwest, and infections might be going unrecognized in these areas. California is increasingly recognized as an area where C. gattii is endemic, and the 13 patients from California could have acquired their infections locally or, perhaps in the case of the California and New Mexico patients with travel to Mexico, in Mexico. The high case-fatality rate indicates a serious public health issue, the scope of which is unknown.
Most patients in this report were otherwise healthy men infected with C. gattii molecular types VGI or VGIII who had CNS disease and positive CSF cultures; fewer patients had positive pulmonary cultures or respiratory symptoms. Many patients had visual disturbances, cranial nerve palsies, and hydrocephalus when seeking treatment or that developed during treatment. Several patients required surgical interventions to mediate persistent elevated ICP. Several patients were treated with corticosteroids, possibly to manage their elevated ICP; clinical treatment guidelines for cryptococcosis recommend judicious use of therapeutic corticosteroids under specific circumstances (13). Cryptococcomas in the lungs and brain were common among patients in this report; these masses are more common among patients with C. gattii than C. neoformans infection (1). These clinical and demographic characteristics, including the disproportionately high number of infected male patients, are similar to those reported for C. gattii infections from other C. gattii–endemic areas of the world, such as Australia and Papua New Guinea, where infections are caused primarily by molecular type VGI (1,2,5–8,22). Most patients in our report received appropriate initial antifungal treatment; of the 2 who died after diagnosis and initiation of treatment, 1 who died 4 days after diagnosis might have received the diagnosis too late for treatment to be effective, and the other died of infection-related causes but not directly from infection. However, 4 patients died before or at diagnosis (and thus before treatment could begin). Three of these 4 had prolonged illness before diagnoses, indicating a likely window of opportunity for earlier diagnosis and treatment that might have led to improved outcomes. Information clearly is needed to determine where in the United States C. gattii infections pose a public health concern and where clinicians need to maintain an elevated index of suspicion for C. gattii infection, particularly for otherwise healthy persons who have signs and symptoms of CNS disease, in whom cryptococcal infection might not be considered in the differential diagnoses.
The clinical signs and symptoms, host characteristics, clinical course, and molecular types of C. gattii infections reported here differ somewhat from those in the US Pacific Northwest outbreak. Most patients with C. gattii in the Pacific Northwest outbreak have underlying, often immunocompromising, medical conditions; are infected with C. gattii molecular types VGIIa, VGIIb, or VGIIc; and have pulmonary symptoms and positive pulmonary cultures (2). Approximately half of the Pacific Northwest patients are female and are a median of 56 years of age (2–13 years older than the median age of patients described here. More than half of patients in the Pacific Northwest outbreak were reported to be taking systemic oral steroids at diagnosis (2), a characteristic not identified among any patients in this report, and few of the patients in that outbreak reported blurred vision or required surgical interventions to mediate persistent elevated ICP during their infections (2).
The reasons for the clinical and demographic differences between outbreak-associated (VGIIa, VGIIb, and VGIIc) and non–outbreak-associated (other molecular types) C. gattii are not clear but may be related to case ascertainment differences, to the molecular type of C. gattii causing infection, to host differences, or a combination of these factors. Some studies have found that a patient’s immune status is critical to the clinical course of cryptococcal infection (1,7,23); for example, HIV-uninfected persons with C. neoformans infections in Asia have more visual and neurologic signs and symptoms consistent with uncontrolled elevated ICP than do HIV-infected patients (23,24). Inflammation can be a defining characteristic of cryptococcal infection in immunocompetent persons (25–27) and might increase the severity of certain symptoms (25,28,29), which accounts for differences in clinical signs and symptoms between the largely immunosuppressed US Pacific Northwest outbreak population and the mostly healthy population reported here. Perhaps the absence (or suppression) of an intact immune response among many C. gattii patients in the Pacific Northwest outbreak increases risk for cryptococcal infection and attenuates its clinical severity by reducing the inflammatory response, thus reducing outcomes such as hydrocephalus and persistent elevated ICP. In contrast, an intact immune response might perversely increase the severity of certain disease symptoms among otherwise healthy C. gattii patients, many of whom reside outside the Pacific Northwest. However, the different strains probably also preferentially infect different patient types, perhaps because of innate requirements of different C. gattii strains. Day et al. and Varma et al. also found that different genetic types of C. neoformans infected immunocompetent and immunocompromised (HIV-infected) persons living in comparable environments and circumstances (30,31); different C. gattii strains might also have predilections for different types of patients. Given the apparent correlation observed in the United States between molecular type of reported C. gattii infections and patient immune status, disentangling these characteristics might be difficult. All of the above factors—the site of infection, the strain, and the host—might be interdependent.
Our report has limitations. First, case reporting was carried out only in areas where laboratory staff, clinicians, or state health departments were aware of and interested in participating in CDC C. gattii surveillance. Thus, the distribution of reported C. gattii isolates might not represent the national distribution of C. gattii isolates outside the Pacific Northwest. Second, most infections in this report came from physicians specifically interested in obtaining species information for cryptococcal infections in their patients, usually because they were HIV uninfected; thus, we cannot make inferences about the frequency of C. gattii infections in HIV-infected persons nor the clinical course of C. gattii disease in HIV-infected persons from this report. Case ascertainment among patients in this group was also likely to differ from ascertainment in the Pacific Northwest, and comparisons between patients in each group should be interpreted with care. Additionally, co-existing pulmonary disease among these patients might be underreported. Although clinicians are likely to try to rule out CNS infection in patients with pulmonary cryptococcosis, such as those in the Pacific Northwest, patients with CNS cryptococcosis might be less likely to have pulmonary sites cultured because identifying the site will not influence treatment. Finally, we might have underestimated travel-associated infections; although most C. gattii infections are considered to have an incubation of 2–13 months (3,4), incubations as long as 3 years have been reported (32). Because most C. gattii incubation period data are based on persons exposed in the Pacific Northwest outbreak, and the outbreak is still relatively nascent, longer incubation periods might manifest as the time since exposure to the outbreak-affected region lengthens.
Although this case series might represent an emerging public health issue in states outside the US Pacific Northwest, it also might represent previously unrecognized disease in these states. Individual clinicians submitted multiple cases for this report, which suggests hotspots of environmental colonization, hotspots of individual interest, or both. However, C. gattii infections have been documented, albeit rarely, in at least some of these areas of the United States: in addition to the few cases identified in southern California, where C. gattii previously has been thought to be endemic, and Hawaii (9,10,14,15,33), a small number of cases also were reported in Georgia (19,33,34). Unlike the clonal outbreak strains found in the Pacific Northwest, the diversity and lack of clonality among the VGI and VGIII isolates from patients reported here indicates that these pathogens most likely have been propagating and diversifying in the United States for a long time. Anecdotal information about and treatment guidelines for C. gattii, primarily based on cases from Australia and Papua New Guinea, suggest that C. gattii infections might require more aggressive or longer treatment than C. neoformans infections (1,7,8,12,13).
An increased index of suspicion for C. gattii infection may be warranted in some areas of the United States; recognition of species gattii infection and early diagnosis might improve outcomes. Species identification of cryptococcal isolates requires specialized agar; however, most clinical laboratories do not identify isolates to the species level. Routine surveillance and species and molecular type identification for C. gattii outside the Pacific Northwest would enable identification of the true range of infections, and shed light on where diagnostics for C. gattii would be most useful.
Dr Harris is an epidemiologist with the Mycotic Diseases Branch at CDC. Her primary research interests include the epidemiology and pathogenesis of C. gattii and other emerging fungal infections.
Acknowledgment
We thank Joyce Peterson and Naureen Iqbal for species identification and DNA fingerprinting of isolates; California local clinicians and communicable disease controllers of Contra Costa, Fresno, Kern, Los Angeles, Orange, San Bernardino, and Santa Clara Counties; Peter Pappas, John Baddley, Jose Vasquez, Sam Lee, Carla Walraven, Likita Aminu, Larry Eron, and Kieren Marr for case referral and submission of case reports to CDC; and Kaitlin Benedict for critical manuscript review.
References
- Chen S, Sorrell T, Nimmo G, Speed B, Currie B, Ellis D, Epidemiology and host- and variety-dependent characteristics of infection due to Cryptococcus neoformans in Australia and New Zealand. Australasian Cryptococcal Study Group. Clin Infect Dis. 2000;31:499–508 and. DOIPubMedGoogle Scholar
- Harris JR, Lockhart SR, Debess E, Marsden-Haug N, Goldoft M, Wohrle R, Cryptococcus gattii in the United States: clinical aspects of infection with an emerging pathogen. Clin Infect Dis. 2011;53:1188–95 and. DOIPubMedGoogle Scholar
- MacDougall L, Fyfe M. Emergence of Cryptococcus gattii in a novel environment provides clues to its incubation period. J Clin Microbiol. 2006;44:1851–2 and. DOIPubMedGoogle Scholar
- Georgi A, Schneemann M, Tintelnot K, Calligaris-Maibach RC, Meyer S, Weber R, Cryptococcus gattii meningoencephalitis in an immunocompetent person 13 months after exposure. Infection. 2009;37:370–3 and. DOIPubMedGoogle Scholar
- Galanis E, Macdougall L. Epidemiology of Cryptococcus gattii, British Columbia, Canada, 1999–2007. [Erratum in: Emerg Infect Dis. 2011;7:1784. Erratum in: Emerg Infect Dis. 2010 16:750]. Emerg Infect Dis. 2010;16:251–7. DOIPubMedGoogle Scholar
- Lalloo D, Fisher D, Naraqi S, Laurenson I, Temu P, Sinha A, Cryptococcal meningitis (C. neoformans var. gattii) leading to blindness in previously healthy Melanesian adults in Papua New Guinea. Q J Med. 1994;87:343–9 .PubMedGoogle Scholar
- Mitchell DH, Sorrell TC, Allworth AM, Heath CH, McGregor AR, Papanaoum K, Cryptococcal disease of the CNS in immunocompetent hosts: influence of cryptococcal variety on clinical manifestations and outcome. Clin Infect Dis. 1995;20:611–6 and. DOIPubMedGoogle Scholar
- Speed B, Dunt D. Clinical and host differences between infections with the two varieties of Cryptococcus neoformans. Clin Infect Dis. 1995;21:28–34 and. DOIPubMedGoogle Scholar
- Kwon-Chung KJ, Bennett JE. Epidemiologic differences between the two varieties of Cryptococcus neoformans. Am J Epidemiol. 1984;120:123–30 .PubMedGoogle Scholar
- Kwon-Chung KJ, Bennett JE. High prevalence of Cryptococcus neoformans var. gattii in tropical and subtropical regions. Zentralbl Bakteriol Mikrobiol Hyg [A]. 1984;257:213–8 .PubMedGoogle Scholar
- López-Martínez R, Soto-Hernández JL, Ostrosky-Zeichner L, Castanón-Olivares LR, Angeles-Morales V, Sotelo J. Cryptococcus neoformans var. gattii among patients with cryptococcal meningitis in Mexico. First observations. Mycopathologia. 1996;134:61–4 and. DOIPubMedGoogle Scholar
- Perfect JR, Dismukes WE, Dromer F, Goldman DL, Graybill JR, Hamill RJ, Clinical practice guidelines for the management of cryptococcal disease: 2010 update by the infectious diseases society of America. Clin Infect Dis. 2010;50:291–322 and. DOIPubMedGoogle Scholar
- Brandt ME, Hutwagner LC, Klug LA, Baughman WS, Rimland D, Graviss EA, Molecular subtype distribution of Cryptococcus neoformans in four areas of the United States. Cryptococcal Disease Active Surveillance Group. J Clin Microbiol. 1996;34:912–7 .PubMedGoogle Scholar
- Chaturvedi S, Dyavaiah M, Larsen RA, Chaturvedi V. Cryptococcus gattii in AIDS patients, southern California. Emerg Infect Dis. 2005;11:1686–92 and. DOIPubMedGoogle Scholar
- Byrnes EJ III, Bildfell RJ, Frank SA, Mitchell TG, Marr KA, Heitman J. Molecular evidence that the range of the Vancouver Island outbreak of Cryptococcus gattii infection has expanded into the Pacific Northwest in the United States. J Infect Dis. 2009;199:1081–6 and. DOIPubMedGoogle Scholar
- Klein KR, Hall L, Deml SM, Rysavy JM, Wohlfiel SL, Wengenack NL. Identification of Cryptococcus gattii by use of
L -canavanine glycine bromothymol blue medium and DNA sequencing. J Clin Microbiol. 2009;47:3669–72 and. DOIPubMedGoogle Scholar - Meyer W, Aanensen DM, Boekhout T, Cogliati M, Diaz MR, Esposto MC, Consensus multi-locus sequence typing scheme for Cryptococcus neoformans and Cryptococcus gattii. Med Mycol. 2009;47:561–70 and. DOIPubMedGoogle Scholar
- Sellers B, Hall P, Cine-Gowdie S, Hays AL, Patel K, Lockhart SR, Cryptococcus gattii: an emerging fungal pathogen in the southeastern United States. Am J Med Sci. 2012;343:510–1 and. DOIPubMedGoogle Scholar
- Walraven CJ, Gerstein W, Hardison SE, Wormley F, Lockhart SR, Harris JR, Fatal disseminated Cryptococcus gattii infection in New Mexico. PLoS ONE. 2011;6:e28625 and. DOIPubMedGoogle Scholar
- Kunadharaju R, Choe U, Harris JR, Lockhart SR, Greene JN. Cryptococcus gattii, Florida, USA, 2011. Emerg Infect Dis. 2013;19:519–21 and. DOIPubMedGoogle Scholar
- Sorrell T, Chen SA, Phillips P, Marr K. Clinical perspectives on Cryptococcus neoformans and Cryptococcus gattii: implications for diagnosis and management. In: Heitman J, Kozel TR, Kwon-Chung J, Perfect J, Casadevall A, editors. Cryptococcus: from pathogen to model yeast. Washington (DC): ASM Press; 2011. p. 595–606.
- Chau TT, Mai NH, Phu NH, Nghia HD, Chuong LV, Sinh DX, A prospective descriptive study of cryptococcal meningitis in HIV uninfected patients in Vietnam—high prevalence of Cryptococcus neoformans var grubii in the absence of underlying disease. BMC Infect Dis. 2010;10:199 and. DOIPubMedGoogle Scholar
- Liao CH, Chi CY, Wang YJ, Tseng SW, Chou CH, Ho CM, Different presentations and outcomes between HIV-infected and HIV-uninfected patients with cryptococcal meningitis. J Microbiol Immunol Infect. 2012;45:296–304 and. DOIPubMedGoogle Scholar
- Ecevit IZ, Clancy CJ, Schmalfuss IM, Nguyen MH. The poor prognosis of central nervous system cryptococcosis among nonimmunosuppressed patients: a call for better disease recognition and evaluation of adjuncts to antifungal therapy. Clin Infect Dis. 2006;42:1443–7 and. DOIPubMedGoogle Scholar
- Einsiedel L, Gordon DL, Dyer JR. Paradoxical inflammatory reaction during treatment of Cryptococcus neoformans var. gattii meningitis in an HIV-seronegative woman. Clin Infect Dis. 2004;39:e78–82 and. DOIPubMedGoogle Scholar
- Lui G, Lee N, Ip M, Choi KW, Tso YK, Lam E, Cryptococcosis in apparently immunocompetent patients. QJM. 2006;99:143–51 and. DOIPubMedGoogle Scholar
- Lane M, McBride J, Archer J. Steroid responsive late deterioration in Cryptococcus neoformans variety gattii meningitis. Neurology. 2004;63:713–4 and. DOIPubMedGoogle Scholar
- Seaton RA, Verma N, Naraqi S, Wembri JP, Warrell DA. The effect of corticosteroids on visual loss in Cryptococcus neoformans var. gattii meningitis. Trans R Soc Trop Med Hyg. 1997;91:50–2 and. DOIPubMedGoogle Scholar
- Day JN, Hoang TN, Duong AV, Hong CT, Diep PT, Campbell JI, Most cases of cryptococcal meningitis in HIV-uninfected patients in Vietnam are due to a distinct amplified fragment length polymorphism-defined cluster of Cryptococcus neoformans var. grubii VN1. J Clin Microbiol. 2011;49:658–64 and. DOIPubMedGoogle Scholar
- Varma A, Swinne D, Staib F, Bennett JE, Kwon-Chung KJ. Diversity of DNA fingerprints in Cryptococcus neoformans. J Clin Microbiol. 1995;33:1807–14 .PubMedGoogle Scholar
- Johannson KA, Huston SM, Mody CH, Davidson W. Unique features of Cryptococcus gattii pneumonia—a prolonged incubation period in an immunocompetent host. Am J Respir Crit Care Med. 2011.
- Bennett JE, Kwon-Chung KJ, Howard DH. Epidemiologic differences among serotypes of Cryptococcus neoformans. Am J Epidemiol. 1977;105:582–6 .PubMedGoogle Scholar
- Denton JF, Di Salvo AF. The prevalence of Cryptococcus neoformans in various natural habitats. Sabouraudia. 1968;6:213–7. DOIPubMedGoogle Scholar
Figure
Tables
Follow Up
Earning CME Credit
To obtain credit, you should first read the journal article. After reading the article, you should be able to answer the following, related, multiple-choice questions. To complete the questions (with a minimum 70% passing score) and earn continuing medical education (CME) credit, please go to www.medscape.org/journal/eid. Credit cannot be obtained for tests completed on paper, although you may use the worksheet below to keep a record of your answers. You must be a registered user on Medscape.org. If you are not registered on Medscape.org, please click on the New Users: Free Registration link on the left hand side of the website to register. Only one answer is correct for each question. Once you successfully answer all post-test questions you will be able to view and/or print your certificate. For questions regarding the content of this activity, contact the accredited provider, CME@medscape.net. For technical assistance, contact CME@webmd.net. American Medical Association’s Physician’s Recognition Award (AMA PRA) credits are accepted in the US as evidence of participation in CME activities. For further information on this award, please refer to http://www.ama-assn.org/ama/pub/category/2922.html. The AMA has determined that physicians not licensed in the US who participate in this CME activity are eligible for AMA PRA Category 1 Credits™. Through agreements that the AMA has made with agencies in some countries, AMA PRA credit may be acceptable as evidence of participation in CME activities. If you are not licensed in the US, please complete the questions online, print the certificate and present it to your national medical association for review.
Article Title:
Cryptococcus gattii infections in Multiple States Outside the US Pacific Northwest
CME Questions
1. You are asked to see a 40-year-old man with neurologic and pulmonary symptoms for the past several weeks. He had received treatment with azithromycin from an urgent care clinic, with no improvement. You consider whether this patient may have a fungal infection. Which of the following statements regarding Cryptococcus gattii infections is most accurate?
A. Transmission is primarily person-to-person
B. The incubation period is approximately 2 to 4 weeks
C. C. gattii primarily affects persons with HIV infection
D. There has been an outbreak of C. gattii in the Pacific Northwest United States
2. What should you consider regarding the presentation of patients with C. gattii infection in the current study?
A. Almost two-thirds of patients were healthy at the time of diagnosis
B. Half of patients were asymptomatic at the time of diagnosis
C. The average time from symptom onset to the diagnosis of C. gattii infection was 3 months
D. Cough and weight loss were the most common presenting symptoms
3. The patient is diagnosed with C. gattii infection of both the lungs and central nervous system. What should you consider regarding the management of patients with C. gattii infection in the current study?
A. Most patients did not require hospitalization
B. There were no admissions to the intensive care unit associated with C. gattii infection
C. Monotherapy with fluconazole was the most common treatment used
D. Over 35% of patients treated for C. gattii infection received corticosteroids
4. What should you consider regarding outcomes of patients with C. gattii infection in the current study?
A. The overall mortality rate exceeded 50%
B. All patients who died had underlying immunocompromised status
C. Nearly 40% of patients with follow-up data had cranial nerve palsies
D. Nearly all patients who died were men
Activity Evaluation
|
1. The activity supported the learning objectives. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
2. The material was organized clearly for learning to occur. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
3. The content learned from this activity will impact my practice. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
4. The activity was presented objectively and free of commercial bias. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
Related Links
Table of Contents – Volume 19, Number 10—October 2013
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Julie R. Harris, Centers for Disease Control and Prevention, 1600 Clifton Rd NE, Mailstop A06, Atlanta, GA 30333, USA
Top