Stockpiling Ventilators for Influenza Pandemics
Hsin-Chan Huang
1
, Ozgur M. Araz, David P. Morton, Gregory P. Johnson, Paul Damien, Bruce Clements, and Lauren Ancel Meyers
Author affiliations: The University of Texas at Austin, Austin, Texas, USA (H.-C. Huang, G.P. Johnson, P. Damien, L.A. Meyers); University of Nebraska, Lincoln, Nebraska, USA (O.M. Araz); University of Nebraska Medical Center, Omaha, Nebraska, USA (O.M. Araz); Northwestern University, Evanston, Illinois, USA (D.P. Morton); Department of State Health Services, Austin (B. Clements); Santa Fe Institute, Santa Fe, New Mexico, USA (L.A. Meyers)
Main Article
Figure 2
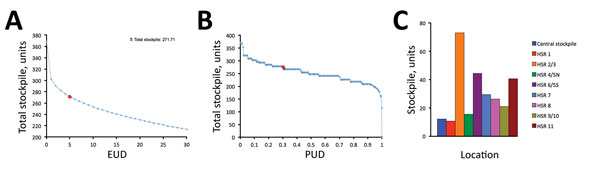
Figure 2. Optimal ventilator stockpiles for a mild pandemic scenario, Texas, USA. The total size of the optimal stockpile, summed across the central and 8 HSR stockpiles, decreases as risk tolerance increases. Risk for unmet demand for ventilators is quantified as the expected number of hospitalized influenza patients statewide not receiving necessary ventilation (EUD) (A) and the probability of at least 1 hospitalized patient in Texas not receiving necessary ventilation (PUD) (B). We optimized directly for EUD and calculated PUD post hoc. Red circles indicate EUD/PUD of 5 patients. C) Optimal allocation among central and regional sites when EUD is set to 5 patients, equivalent to a stockpile of 272 ventilators. EUD, expected unmet demand; PUD, probability of unmet demand; HSR, health service region.
Main Article
Page created: May 30, 2017
Page updated: May 30, 2017
Page reviewed: May 30, 2017
The conclusions, findings, and opinions expressed by authors contributing to this journal do not necessarily reflect the official position of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors' affiliated institutions. Use of trade names is for identification only and does not imply endorsement by any of the groups named above.
