Volume 28, Number 4—April 2022
Research Letter
Multisystem Inflammatory Syndrome in Adult after First Dose of mRNA Vaccine
Abstract
A 32-year-old man in Japan experienced respiratory failure after receiving the first dose of coronavirus disease (COVID-19) vaccine. He was treated with noninvasive ventilation and corticosteroids. Serologic test results suggested previous COVID-19; therefore, he received a diagnosis of multisystem inflammatory syndrome. COVID-19 vaccination could be a trigger for this condition.
A 32-year-old man from France living in Tokyo was admitted to the National Center for Global Health and Medicine after experiencing shortness of breath and fever. He had received the first dose of the BNT162b2 (Pfizer-BioNTech, https://www.pfizer.com) vaccine 5 days before admission. After vaccination, he experienced a fever, systemic joint pain, nausea, and vomiting. The patient sought care because of these persistent symptoms.
At admission, the patient was experiencing dyspnea as well as chest and back pain that worsened during inhalation. The patient was obese (body mass index 42.1 kg/m2). He had no history of smoking, illegal drug use, or international travel. When he received the vaccine, Japan was experiencing its largest coronavirus disease (COVID-19) surge, but he had no known exposure to patients with COVID-19. At admission, he had a body temperature of 38.1°C and peripheral oxygen saturation (SpO2) of 95% on room air (Table). He had no notable jugular venous dilation, chest crackles, peripheral edema, or rashes.
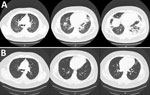
Laboratory test results showed an elevated inflammatory response and cardiac enzymes (Table). Chest computed tomography (CT) showed smooth interlobular septal thickening, mixed lesions with ground-glass opacitie, and infiltrates in the bilateral lower lobes (Figure, panel A). Electrocardiography showed slight ST segment elevations in leads I, aVL, V1, and V2. Echocardiography showed no pericardial effusion, myocardial edema, or decreased wall motion. Real-time PCR results were negative for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Loop-mediated isothermal amplification did not detect Legionella pneumophila. We used FilmArray version 1.3 (bioMérieux, https://www. biomerieux.com) to conduct a respiratory panel on respiratory specimens and a meningitis/encephalitis panel on serum specimens to detect herpesvirus, enterovirus, and cytomegalovirus; results of both panels were negative.
One day after admission, the patient’s dyspnea and hypoxemia worsened, and he experienced profuse cold sweats. His SpO2 dropped to 90% despite 10 L/min of oxygen supply. We suspected severe respiratory failure resulting from COVID-19 vaccine–related systemic inflammation and congestive heart failure. Therefore, we treated the patient with intravenous methylprednisolone at a dose of 1 mg/kg/day (125 mg/d) and with diuretics and noninvasive ventilation (NIV). The next day, his symptoms and hypoxemia greatly improved. He tapered off both treatments; he no longer needed ventilation 2 days after treatment and completed the course of steroids by the day of discharge, 7 days after admission. One month after discharge, CT was performed to confirm the improvement in the lung lesions (Figure, panel B).
Testing showed that SARS-CoV-2 spike IgG and neutralizing activities were significantly elevated 5 days and 23 days after the first COVID-19 vaccination dose had been administered (Appendix Figure 1). Moreover, SARS-CoV-2 nucleocapsid IgG in the serum was positive 5 days after COVID-19 vaccination. On the basis of these findings, we hypothesize that the patient had an asymptomatic or mild SARS-CoV-2 infection before vaccination. After his discharge, we measured a panel of 67 cytokines and chemokines from the patient and 3 healthy controls for comparison (Appendix Table, Figure 2).
This case emphasized 2 clinical issues. First, severe respiratory failure can occur after COVID-19 vaccination, and steroids effectively alleviated this complication. Second, multisystem inflammatory syndrome in adults (MIS-A) can occur after COVID-19 vaccination in a previously infected patient and can manifest as respiratory distress. In cases of respiratory failure after the vaccination, a previous SARS-CoV-2 infection should be considered.
Postvaccination myocarditis has been reported as more common in male than female patients (1). Bozkurt et al. described mild cases (1); however, severe cases have also been reported (2). Although our patient’s myocardial damage was not severe, we suspected myocarditis based on his elevated troponin I level after COVID-19 vaccination. Vaccine-related myocarditis typically develops after the second vaccination, but it has been reported after the first vaccination of patients who had COVID-19 previously (1). Therefore, we considered the possibility of myocarditis after the first vaccination in this patient, because his serology results suggested a history of COVID-19. Moreover, his respiratory failure, severe inflammation, and serologic test results strongly suggesting a history of COVID-19 led us to suspect MIS-A, as reported by Morris et al. (3). Although the association between the COVID-19 vaccine and MIS-A development is unclear (4), the patient in our case fulfilled the clinical criteria of severe cardiac illness, hypotension, vomiting, and fever. In addition, his laboratory results showed elevated C-reactive protein levels, ferritin levels, interleukin-6 levels, and erythrocyte sedimentation rate. He also exhibited serologic positivity for SARS-CoV-2. These findings were consistent with the definition of MIS-A (5). This case showed that vaccination was a possible trigger of MIS-A in a patient who had a history of COVID-19.
The treatment for postvaccination myocarditis and MIS-A has not been standardized. As demonstrated in our case, immunosuppressive therapy, particularly corticosteroids, improved the prognosis. Intravenous immunoglobulin, anakinra, and infliximab have been used to treat multisystem inflammatory syndrome in children (6,7); a previous case report documented their role in treating MIS-A (8).
Dr. Miyazato is a clinical fellow in the Disease Control and Prevention Center at the National Center for Global Health and Medicine. His primary research interests are sexually transmitted diseases and clinical infectious diseases.
Acknowledgments
We thank Hitomi Igarashi for providing technical assistance.
This research was supported by the National Center for Global Health and Medicine Intramural Research Fund (grant no. 21A006) and Japan Agency for Medical Research and Development Research Program on Emerging and Re-emerging Infectious Diseases (no. JP20fk0108416).
References
- Bozkurt B, Kamat I, Hotez PJ. Myocarditis with COVID-19 mRNA vaccines. Circulation. 2021;144:471–84. DOIPubMedGoogle Scholar
- Abbate A, Gavin J, Madanchi N, Kim C, Shah PR, Klein K, et al. Fulminant myocarditis and systemic hyperinflammation temporally associated with BNT162b2 mRNA COVID-19 vaccination in two patients. Int J Cardiol. 2021;340:119–21. DOIPubMedGoogle Scholar
- Morris SB, Schwartz NG, Patel P, Abbo L, Beauchamps L, Balan S, et al. Case series of multisystem inflammatory syndrome in adults associated with SARS-CoV-2 infection—United Kingdom and United States, March–August 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1450–6. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Interim clinical considerations for use of COVID-19 vaccines currently approved or authorized in the United States. 2021 [cited 2021 Dec 10]. https://www.cdc.gov/vaccines/covid-19/clinical-considerations/covid-19-vaccines-us.html
- Centers for Disease Control and Prevention. Multisystem inflammatory syndrome in adults (MIS-A) case definition information for healthcare providers. 2021 [cited 2022 Jan 16]. https://www.cdc.gov/mis/mis-a/hcp.html
- Henderson LA, Canna SW, Friedman KG, Gorelik M, Lapidus SK, Bassiri H, et al. American College of Rheumatology clinical guidance for multisystem inflammatory syndrome in children associated with SARS-CoV-2 and hyperinflammation in pediatric COVID-19: version 2. Arthritis Rheumatol. 2021;73:e13–29. DOIPubMedGoogle Scholar
- Cole LD, Osborne CM, Silveira LJ, Rao S, Lockwood JM, Kunkel MJ, et al. IVIG compared with IVIG plus infliximab in multisystem inflammatory syndrome in children. Pediatrics. 2021;148:
e2021052702 . DOIGoogle Scholar - Ahmad F, Ahmed A, Rajendraprasad SS, Loranger A, Gupta S, Velagapudi M, et al. Multisystem inflammatory syndrome in adults: A rare sequela of SARS-CoV-2 infection. Int J Infect Dis. 2021;108:209–11. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleOriginal Publication Date: February 11, 2022
Table of Contents – Volume 28, Number 4—April 2022
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Kei Yamamoto, Disease Control and Prevention Center, National Center for Global Health and Medicine, 1-21-1 Toyama, Shinjuku-ku, Tokyo 162-8655, Japan
Top