Volume 4, Number 4—December 1998
Dispatch
Murine Typhus in Travelers Returning from Indonesia
Abstract
We report the first three documented cases of murine typhus imported into Europe from Indonesia, discuss clues for the diagnosis of the disease, and urge that murine fever be considered in the diagnosis of febrile disease in travelers.
One of the oldest recognized, most common, but least reported arthropod-transmitted zoonoses (1,2), murine virus is caused by Rickettsia typhi, formerly named R. mooseri, a gram-negative obligate intracellular bacterium (1,2). The main vector of murine typhus is the rat flea Xenopsylla cheopis, which maintains R. typhi in rodents. Flea bites and contamination of excoriated skin or the respiratory tract with infected flea feces are the major sources of human infection throughout the world (2). The classic reservoir and vector are the rat and rat flea, respectively (2); however, the role of cat fleas and opossums in maintaining this microorganism has been suggested in some areas of the United States where rats and rat fleas are absent (2,3). Although murine typhus has a worldwide distribution, it is often unrecognized, and documented cases are rarely reported, particularly in tropical countries. Three recent cases of murine typhus in 2 months in patients returning to Europe from Indonesia indicate that murine typhus should be considered a possible cause of imported fever from Indonesia.
In October 1997, a 29-year-old man living in France was hospitalized with a 2-day history of fever. On admission, his temperature was 40°C and his pulse, at 70/min, was dissociated. No signs of eruption or other abnormalities were observed. The patient had returned from a 3-week trip to Bali, Indonesia, 2 weeks before his hospitalization but reported no arthropod bites during his trip. Increases of alanine aminotransferase (110 U/L), aspartate aminotransferase (120 U/L), lactate dehydrogenase (1000 U/L) and reactive protein C (130 mg/L) associated with a low white blood cell count were noted. Repeated blood smears did not disclose any malaria parasites. The patient received a 21-day treatment with doxycycline plus rifampin and became afebrile on day 3. He was discharged from the hospital and remained well. An indirect immunofluorescence assay (IFA) for antibodies reactive with R. typhi antigens (4) showed raised levels of immunoglobulin (Ig) M (1:512) and IgG (1:256).
Case 2
In November 1997, a 28-year-old man living in France was hospitalized with a 6-day history of fever. On admission, he had a low-grade fever (38°C). Physical examination found no abnormalities except for a few skin ulcerations of the inguinal area. The patient had returned from Bali 3 weeks before his hospitalization but reported no arthropod bites during his trip. Biologic findings were unremarkable. Blood smears did not disclose malaria parasites. The blood cell count, hemoglobin level, and blood chemistry values were within normal limits. Serologic testing for antibodies reactive with R. typhi antigens showed raised levels of IgM (1:512) and IgG (1:256).
Case 3
The third patient, a 28-year-old man from Belgium, became acutely ill during a trip to Indonesia (Bali, Lava, Lombok), with a fever (40°C), shivers, diffuse myalgia, but no rash. He was treated in Indonesia with amoxicillin, followed by cefuroxim-axetil (500 mg twice a day for 10 days), without success. The patient recalled multiple insect bites during his trip. Clinical examination on arrival in Belgium showed severe disease with bilateral conjunctivitis and splenomegaly, but no adenopathies. Biologic findings were unremarkable except raised levels of alanine aminotransferase (681 U/L), aspartate aminotransferase (659 U/L), and reactive protein C (17 mg/L). Analysis of the cerebrospinal fluid showed 20 leukocytes/ml with 75% polymorphonuclear cells. Repeated blood smears did not disclose any parasites. The patient received empirical treatment with quinine, doxycycline, and a quinolone to treat suspected malaria or salmonellosis. The fever rapidly resolved, and the patient recovered. Serologic testing with IFA was positive for R. typhi (IgG, 512; IgM, 1024). Antibodies to R. typhi were also detected in the cerebrospinal fluid (IgM, 2).
All patients exhibited serologic cross-reactions (low titers) with R. prowazekii, the agent of epidemic typhus, and R. conorii, the agent of Mediterranean spotted fever (Table;1,4). Serologic findings were completed by cross-absorption. When absorption was performed with R. typhi, homologous and heterologous antibodies disappeared, but when absorption was performed with R. prowazekii, only homologous antibodies disappeared; therefore, murine typhus was diagnosed as the cause of illness in the three patients (4).
Murine typhus is a mild disease with nonspecific signs (1). The incubation period is 7 to 14 days. The classic triad of fever, headache, and skin rash is observed in fewer than 15% of cases (5). While fever and headache are frequent, a rash occurs in only half of the patients and is often transient or unimpressive. This is illustrated in these three cases, where no rash was noted. Arthralgia, myalgia, or respiratory and gastrointestinal symptoms are frequent (5). Leukocytosis and mild leukopenia, anemia, and thrombopenia occur frequently; hyponatremia, hypoalbuminemia, hepatic abnormalities, or renal dysfunction may occur (5). Fewer than half of the patients report exposure to fleas or flea hosts. Of the cases reported here, only one involved insect bites. Untreated patients may have fever and symptoms for 7 to 14 days and then rapidly convalesce. The treatment of choice is antibiotic therapy with tetracyclines. A single 200-mg dose of oral doxycycline usually leads to defervescence during the first 72 hours (6).
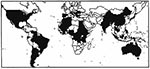
Like our patients, most murine typhus patients may have isolated fever and nonspecific biologic abnormalities. Diagnosis may be missed because the rash, the hallmark of rickettsial diseases, is absent (1). For example, in a recent review in the United States, 22 different diagnoses were proposed for 80 patients with murine typhus (5). Consequently, the diagnosis of the disease is based on serologic testing. The reference method is immunofluorescence; however, a latex test, a dot blot enzyme-linked immunosorbent assay, and an immunoperoxydase assay have also been described (4). The fact that travel-associated cases of murine typhus have been identified and may represent a source of imported fever indicates that serologic testing should be considered in febrile patients returning from disease-endemic areas (Figure).
Tissot-Dupont et al. recently reported that the prevalence of antibodies against R. typhi in humans in Africa was higher in coastal areas where rats are prevalent (Figure; 7). Other seroepidemiologic studies demonstrated substantial seroprevalence in Asia (Thailand, Vietnam, Japan, Indonesia, China), Europe (Croatia, Greece), and Australia (6,8). Cases have recently been reported in Greece, Spain, Portugal, Israel, and Thailand (6). The disease is known to be endemic in the United States (particularly California, Hawaii, and Texas) and Mexico (6). Some authors have reported the disease in Rumania, Yugoslavia, Albania, Italy, areas around the Caspian Sea, in Kuwait, Latin America (Venezuela, Argentina, Brazil, Chile, Ecuador, Panama, Guatemala, Puerto Rico), and French Guyana (9). However, serologic cross-reactivity may occur between R. typhi and R. prowazekii, the agent of epidemic typhus (1,4). Epidemic typhus, transmitted by body lice, occurs more frequently in cool areas where clothes are infrequently changed and particularly during human conflicts (1). The disease is prevalent in countries at high altitudes in Central America or Africa (10,14); interpretation of serologic results in these countries has at times been difficult (7,10). However, cross-absorption is a useful technique for identifying the infecting rickettsia to species level as reported in the present cases (4).
Cases of murine typhus have been reported in travelers returning from India, Nepal, Morocco, Canary Islands, Spain, and Africa (6,11-13). Although a case of murine typhus was reported in a patient after a trip to Malaysia and Indonesia (11), the cases reported here are the first serologically documented cases clearly imported from Indonesia. In Malang, East Java, humans are highly exposed to R. typhi, and murine typhus appears to be endemic in the region (8).
Fever is a common problem in patients returning from travel abroad. Although malaria is often suspected, rickettsial diseases (including murine typhus) are generally not. Our cases indicate that murine typhus should be considered in the diagnosis of febrile illness in travelers returning from disease-endemic areas, particularly if fever is present and blood smears show no malaria parasites. Rickettsial diseases were recently cited as the third most frequent cause of imported fever in Switzerland (12). On the basis of this study and two previous reports from France (13) and the United States (11), murine typhus is a frequently imported rickettsial disease. Increased development of tourism and travel to tropical countries should lead to an increase in the documentation of cases.
Dr. Raoult is affiliated with the hospital of Université de la Méditerranée, in Marseille, France. His research interest is medical entomology.
References
- Raoult D, Roux V. Rickettsioses as paradigms of new or emerging infectious diseases. Clin Microbiol Rev. 1997;10:694–719.PubMedGoogle Scholar
- Azad AF, Radulovic S, Higgins JA, Noden BH, Troyer JM. Flea-borne rickettsioses: ecologic considerations. Emerg Infect Dis. 1997;3:319–27. DOIPubMedGoogle Scholar
- Azad AF, Sacci JB, Nelson WM, Dasch GA, Schmidtmann ET, Carl M. Genetic characterization and transovarial transmission of a typhus-like rickettsia found in cat fleas. Proc Natl Acad Sci U S A. 1992;89:43–6. DOIPubMedGoogle Scholar
- Lascola B, Raoult D. Laboratory diagnosis of rickettsioses: current approaches to diagnosis of old and new rickettsial diseases. J Clin Microbiol. 1997;35:2715–27.PubMedGoogle Scholar
- Dumler JS, Taylor JP, Walker DH. Clinical and laboratory features of murine typhus in South Texas, 1980 through 1987. JAMA. 1991;266:1365–70. DOIPubMedGoogle Scholar
- Walker DH. Advances in understanding of typhus group rickettsial infections. In: Kazar J, Toman R, editors. Rickettsiae and rickettsial diseases. Bratislava, Slovak Republic: VEDA Press; 1996. p. 16-25.
- Tissot-Dupont H, Brouqui P, Faugere B, Raoult D. Prevalence of antibodies to Coxiella burnetii, Rickettsia conorii, and Rickettsia typhi in seven African countries. Clin Infect Dis. 1995;21:1126–33.PubMedGoogle Scholar
- Richards AL, Soeatmadji DW, Widodo MA, Sardjono TW, Yanuwiadi B, Hernowati TE, Seroepidemiologic evidence of murine typhus and scrub typhus in Malang, Indonesia. Am J Trop Med Hyg. 1997;57:91–5.PubMedGoogle Scholar
- Traub R, Wisseman CL Jr, Azad AF. The ecology of murine typhus: a critical review. Trop Dis Bull. 1978;75:237–317.PubMedGoogle Scholar
- Perrine PL, Chandler BP, Krause DK, McCardle P, Awoke S, Habte-Gabr E, A clinico-epidemiological study of epidemic typhus in Africa. Clin Infect Dis. 1992;14:1149–58.PubMedGoogle Scholar
- McDonald JC, MacLean JD, McDade JE. Imported rickettsial disease: clinical and epidemiologic features. Am J Med. 1988;85:799–805. DOIPubMedGoogle Scholar
- Raeber PA, Winteler S, Paget J. Fever in the returned traveller: remember rickettsial diseases. Lancet. 1994;334:331. DOIGoogle Scholar
- Edlinger E, Navarro P. Rickettsioses. A disease of tourism. Sem Hop Paris. 1983;59:2053–4.PubMedGoogle Scholar
- Raoult D, Roux V, Ndihokubwayo JB, Bise G, Baudon D, Marte G, Jail fever (epidemic typhus) outbreak in Burundi. Emerg Infect Dis. 1997;3:357–60. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleTable of Contents – Volume 4, Number 4—December 1998
| EID Search Options |
|---|
|
|
|
|
|
|