Volume 8, Number 12—December 2002
Synopsis
Antimicrobial Resistance in Streptococcus pneumoniae, Taiwan
Abstract
Taiwan has one of the highest levels of antibiotic-resistant pneumococcus in the world. Pneumococcal isolates not susceptible to penicillin first appeared in Taiwan in 1986; in 1995 an increase in the prevalence of nonsusceptibility to penicillins, extended-spectrum cephalosporins, trimethoprim-sulfamethoxazole, and macrolides as well as multidrug resistance began to be recognized. With the persistence of antibiotic selective pressure, resistance in some antibiotics reached a high plateau (β-lactam antibiotics) or continued to increase (macrolides), while novel resistance (fluoroquinolones) emerged in the last 3 years. Widespread distribution of some novel resistant 23F and 19F clones (and the international epidemic of 23F clones) contributes further to the rapid increase of resistance. Because Streptococcus pneumoniae is a major pathogen that causes community-acquired lower respiratory tract infections and meningitis in adults and children, antibiotic-resistance in this organism is a serious problem.
For more than a century, Streptococcus pneumoniae has been known as the major bacterial pathogen in humans, causing substantial illness and death (1,2). Before 1967, this organism was uniformly susceptible to penicillin. In the early 1990s, pneumococcal isolates appeared that exhibited a high level of resistance to penicillin and other β-lactam antibiotics (1). The widespread emergence of this resistance in many countries has become a major concern in recent years. The persistence of high antibiotic selective pressure in the community and international spread of epidemic or countrywide circulation of endemic multiresistant clones have substantially contributed to the crisis of resistance (3). This resistance has complicated treatment options and increased the likelihood of treatment failure (2).
The Asian region is one of the epicenters for pneumococcal resistance, and Taiwan has become the focus of pneumococcal resistance since 1996, particularly after several reports documented the alarmingly high prevalence among clinical isolates of resistance to β-lactam antibiotics and macrolides (4–12). The Center for Disease Control under the Department of Health in Taiwan established an active surveillance program in 1998 to study the epidemiologic features of invasive pneumococcal diseases in Taiwan. Furthermore, a nationwide surveillance system for antimicrobial resistance involving 12 major teaching hospitals (Surveillance from Multicenter Antimicrobial Resistance in Taiwan [SMART]) has also tracked the trends of pneumococcal resistance annually since 2000. In this report, we will discuss the trends of pneumococcal resistance, evidence of dissemination of resistant clones, and substantial community use of antibiotics, and highlight critical resistance problems.
The incidence of invasive infections caused by S. pneumoniae in Taiwan is still unknown, although several studies regarding invasive pneumococcal infections in adults and children have been reported (9,13–19). The overall mortality rate (42.5%) for elderly patients (>65 years of age) with invasive infections (bacteremia, pneumonia, pleural empyema, meningitis, septic arthritis, and peritonitis) was higher than the rates for patients 19–64 years of age (22.4%) and for children (8.1%) (9). Some factors, such as the presence of serotype 3 strain, shock as initial presentation, and multilobar pneumonia, were significantly associated with death from invasive infections (14,15). Another report from central Taiwan indicated that the overall mortality rate for children with invasive pneumococcal infections was 20.3%, and in 53.3%, the infections progressed rapidly to death (18). Other studies found that 70% to 80% of adult patients with invasive pneumococcal disease had underlying diseases (malignancies, followed by congestive heart failure and diabetes mellitus) (14,15). Patients with HIV infection or multiple myeloma in whom invasive pneumococcal infection developed were extremely rare (14,13–20). No significant difference was found in the mortality rates of patients with penicillin-susceptible (PSSP) and those with penicillin-nonsusceptible S. pneumoniae (PNSSP) infections (9,14,15,18).
The prevalence of this organism that causes community-acquired pneumonia or meningitis in adults or children is obscure. Several reports have indicated that this organism causes 19% to 33% of infections that results in bacterial meningitis in children (21–23). In one study of adult patients, 28% of the community-acquired bacterial meningitis were caused by S. pneumoniae, the highest proportion after that was by Klebsiella pneumoniae (33%) (24). The incidence (cases per 100,000 emergency visits) of pneumococcal meningitis at National Taiwan University Hospital was 2.8 in 1997–1998 (24). In other study, S. pneumoniae accounted for 21.8% of bacterial pathogens isolated from middle ear fluid from 243 children with acute otitis media (25).
Resistance to Penicillin and Other β-lactam Antibiotics
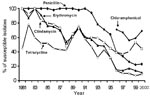
The first clinical isolate of S. pneumoniae not susceptible to penicillin (MIC, >2 μg/mL) was reported in 1986 (26). At National Taiwan University Hospital, a clinical isolate of PNSSP might have also been first seen in 1986 (the disk used for determining penicillin susceptibility was not the standard 1-μg disk). A stepwise decline in the annual rates of susceptibilities to penicillin from 1981 to 2000 at National Taiwan University Hospital (disk susceptibility data from all sites of isolates) (Figure 1) and a high prevalence (60%–84%) of clinical PNSSP isolates were noted throughout the island (disk susceptibility data from all sites of isolates) (12).
The table summarizes the results of dilution susceptibility tests for S. pneumoniae isolated from various clinical specimens (6–8, 10) and normally sterile sites (9) of patients seen from 1996 to 2000. The results were similar to those determined by the disk diffusion method (12). The proportions of high-level resistance to penicillin (MIC >2 μg/mL) varied from 8% to 33%; however, isolates exhibiting an MIC of penicillin of <4 μg/mL accounted for <12%. About 60% of isolates with intermediate resistance to penicillin also had intermediate resistance to cefotaxime or ceftriaxone, and nearly all isolates resistant to penicillin were also not susceptible to those two agents (6–9). The resistance level was higher among nasopharyngeal isolates from colonized children (71%) or among isolates from children with invasive conditions (such as bacteremia, pneumonia, meningitis, peritonitis, and empyema thoracis) than those from adults with invasive conditions (76% vs. 45%) (chi-square test, p=0.0000009) (5,9). About 50% of isolates from blood or cerebrospinal fluid samples were not susceptible to penicillin ( 6,7,9). Among isolates recovered from patients hospitalized in the intensive care units from five major teaching hospitals in Taiwan, 58% were not susceptible to penicillin, 33% were not susceptible to cefotaxime, and 21% showed intermediate resistance to imipenem (10).
Resistance to Macrolides
A similar trend of decreased annual rates of susceptibility for S. pneumoniae was also observed in erythromycin. (Table and Figure 1). Overall, the prevalence of clinical isolates of S. pneumoniae not susceptible to erythromycin was 67% to 100% island-wide (12). Only about one-third of the erythromycin-resistant isolates exhibited M-phenotype (27).
Resistance to Fluorquinolones or Other Antibiotics
Isolates not susceptible to ciprofloxacin (MIC >4 μg/mL) might have first been noted in 1996, but the first clinical isolate that was highly resistant to ciprofloxacin (MIC >32 μg/mL) and other newer fluoroquinolones was documented in 1999 (6,8,28,29). This isolate had mutations in genes gyrA and parC and also possessed an efflux mechanism (28). Isolates not susceptible to trimethoprim-sulfamethoxazole accounted for 60% to 90% (6–10). All isolates are susceptible to vancomycin and linezolid, but some strains were resistant to quinupristin-dalfopristin (10,29). More than 90% of PNSSP isolates were also resistant to multiple antibiotics (resistant to at least three classes of antibiotics) (6–10).
Several factors limit our conclusions regarding the trends of pneumococcal resistance in Taiwan. First, data on antibiotic resistance gained from disk diffusion testing in some studies are not optimal because such studies tend to overestimate penicillin resistance compared with estimates determined by the dilution method. Second, studies that report resistance data of a mixture of invasive and noninvasive isolates and of isolates from different location for different years make it hard to assess the trends over time since resistance may vary with sites of isolates and geographic location. Third, resistance data from one hospital cannot be compared with data from larger populations since single hospitals may have more referral bias for severe cases and do not necessarily represent the phenomenon of the larger population.
Spread of Resistant Clones
Although one report has supported the idea that the international epidemic (Spanish 23F) clone was introduced and diffused in Taiwan (30), multiple domestic and novel clones (23F, 19F, and 6B), which have exhibited high-level resistance to penicillin, extended-spectrum cephalosporins, and macrolides, continuously circulate in our community (9,31,32). Two penicillin-resistant clones that acquired separate mechanisms of macrolide resistance, i.e. Taiwan-23F clone isolates exhibiting high-level resistance to erythromycin with an MIC of >256 μg/mL (ermAM genes mediated) and Taiwan-19F clone isolates with erythromycin resistance shown by an MIC of 1.5–8 μg/mL (mefE gene–mediated), have already spread (30). Isolates belonging to the same clone caused various invasive diseases of different patients who lived in different parts of Taiwan, and resulted in bacteremic pneumonia in siblings (9,31,33). The spread of an endemic and highly resistant 23F clone (penicillin MIC, 4 μg/mL and erythromycin MIC, >256 μg/mL) in one day care center was also reported (34). The spread of Taiwan clones to other parts of the world (Taiwan 19F-14 and Taiwan-6B clones to Hong Kong and United Kingdom; Taiwan 19F-14 to the United States) has also been documented (30, 35, 36). Although the dissemination of fluoroquinolone-resistant strains has been documented in Hong Kong and Brooklyn, New York (37,38), to date, the clonal spread of these resistant strains has not been found in Taiwan.
A high dose of intravenous penicillin G is still recommended as one of the primary drugs of choice for the empirical treatment of patients with community-acquired pneumonia who need hospitalization because about 10% of our clinical isolates have an MIC of penicillin of ≥4 μg/mL (6–10,39). MIC testing, mostly by the E-test, for penicillin-nonusceptible (oxacillin 1-μg disk) isolates recovered from respiratory secretion or blood specimens from patients without meningitis, is always performed in most teaching hospitals in Taiwan (39, 40). Obviously, the guidelines for the treatment of community-acquired pneumonia in adults recommended by the American Thoracic Society in 2001 (41) and the Infectious Diseases Society of America in 2000 (42), as well as suggestions for the management of sinusitis, otitis media, and chronic bronchitis, which include one macrolide alone as the drug of choice or as an alternative antimicrobial agent, are inappropriate in Taiwan. This is because of the high incidence of macrolide resistance and the high proportion of MLSB-phenotype among these resistant isolates.
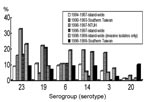
Figure 2 illustrates the distribution of six major serogroups or serotypes of S. pneumoniae isolates from 1984 to 1998 (4,6,7,9,19,43). The frequencies of serogroups (serotypes) 23 (23F) and 19 (19F) increased remarkably, whereas those of serotypes 14, 3, and 1 declined. Some unusual serotypes (serotypes 20, 11, 7, and 8) appeared to emerge in southern Taiwan. No relationship was found between the serogroup or serotype distribution of isolates and the patients’ ages (p >0.05) (6,7,9). PNSSP exhibited resistance to isolates from various serogroupsor serotypes. Among them, serogroups 11 and 23 isolates had the highest incidence of penicillin nonsusceptibility and multidrug resistance. However, serotype 3 isolates (0%–22%) and serotype 20 (11%) isolates had lower rates of nonsusceptibility to penicillin (4,6,9,19). In general, more than 90% of isolates causing invasive infections were included in the serogroups or serotypes covered by the 23-valent pneumococcal and 7-valent conjugate vaccine (4,9).
Before 1995, few regulations regarding antibiotic use existed for physicians in primary care clinics or hospitals. Furthermore, many antibiotics could easily be obtained at drugstores without a prescription. Although the medical payment has been regulated by the National Health Insurance program, implemented in Taiwan in 1995, antibiotics are still commonly used and seem to be overprescribed in primary care units (44). From 1996 to 1999, about 12% to 14% of total patient-visits in primary care units had antibiotic use. The common cold (32.3%) was the most frequent diagnosis for which antibiotics were prescribed. Penicillins (35.4%), cephalosporins (26.5%), and macrolides (21.6%) were the most commonly prescribed classes of antibiotics (44). In 1999, a reported point prevalence rate of about 7.5% among healthy high school students and healthy ambulatory elderly persons who had antimicrobial activity in their urine suggested that this may be the baseline for antibiotic use in the community (45). Surprisingly, over half of the patients who came to the emergency department of a large teaching hospital in Taiwan had taken antibiotics within the previous 12–48 hours. With the increasing and highly selective pressure of antibiotic usage in our community, the crisis of resistance continues to exist.
In the new millennium, the Center for Disease Control under the Department of Health in Taiwan has made nationwide surveillance of antimicrobial resistance and strict control of antibiotic usage major tasks. The new regulations for antibiotic prescription, established by the Bureau of National Health Insurance in 2001 (44), restrict the inappropriate use of the so-called first-line antibiotics (first-generation cephalosporins, macrolides, and gentamicin) for treating various infections, particularly the trivial upper respiratory tract infection. The use of the 23-valent pneumococcal vaccine, especially among high-risk adults and older persons, is encouraged, and new protein-conjugate vaccines will be introduced in the near future.
Taiwan has one of the highest levels of antibiotic resistant pneumococcus in the world. With the increase in international travel, the interchange of resistant clones among countries is unavoidable and the widespread distribution of these clones is expected. Strategies to limit the upsurge of resistant pneumococcus include improved surveillance, reduced antibiotic usage, and increased vaccination of persons at high risk. The judicious use of antimicrobial agents is necessary to avoid providing a selective advantage for resistant organisms. The active surveillance of resistant organisms can help track local resistance problems, prevent the future dissemination of these organisms, and provide options appropriate for empiric therapy.
Dr. Hsueh is an assistant professor in the departments of Laboratory Medicine and Internal Medicine, National Taiwan University Hospital, National Taiwan University College of Medicine. His research interests include mechanisms of antimicrobial resistance and molecular epidemiology of emerging pathogens. He is actively involved in a national research program for antimicrobial drug resistance, Surveillance for Multicenter Antimicrobial Resistance in Taiwan (SMART).
References
- Appelbaum PC. Antimicrobial resistance in Streptococcus pneumoniae: an overview. Clin Infect Dis. 1992;15:77–83.PubMedGoogle Scholar
- Kaplan SL, Mason EO Jr. Management of infections due to antibiotic-resistant Streptococcus pneumoniae. Clin Microbiol Rev. 1998;11:628–44.PubMedGoogle Scholar
- Muñoz R, Coffey TC, Daniels M, Dowson CG, Labible G, Casal J, Intercontinental spread of a multiresistant clone of serotype 23F Streptococcus pneumoniae. Clin Infect Dis. 1992;15:112–8.PubMedGoogle Scholar
- Hsueh PR, Chen HM, Lu YC, Wu JJ. Antimicrobial resistance and serotype distribution of Streptococcus pneumoniae strains isolated in southern Taiwan. J Formos Med Assoc. 1996;95:29–36.PubMedGoogle Scholar
- Chiou CC, Liu YC, Huang TS, Hwang WK, Wang JH, Lin HH, Extremely high prevalence of nasopharyngeal carriage of penicillin-resistant Streptococcus pneumoniae among children in Kaohsiung, Taiwan. J Clin Microbiol. 1998;36:1933–7.PubMedGoogle Scholar
- Hsueh PR, Teng LJ, Lee LN, Yang PC, Ho SW, Luh KT. Extremely high incidence of macrolide and trimethoprim-sulfamethoxazole resistance among clinical isolates of Streptococcus pneumoniae in Taiwan. J Clin Microbiol. 1999;37:897–901.PubMedGoogle Scholar
- Fung CP, Hu BS, Lee SC, Liu PY, Jang TN, Leu HS, Antimicrobial resistance of Streptococcus pneumoniae isolated in Taiwan:an island-wide surveillance study between 1996 and 1997. J Antimicrob Chemother. 2000;45:49–55. DOIPubMedGoogle Scholar
- Hsueh PR, Liu YC, Shyr JM, Wu TL, Yan JJ, Wu JJ, Multicenter surveillance of antimicrobial resistance of Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis in Taiwan during the 1998–1999 respiratory season. Antimicrob Agents Chemother. 2000;44:1342–5. DOIPubMedGoogle Scholar
- Siu LK, Chu ML, Ho M, Lee YS, Wang CC. Epidemiology of invasive pneumococcal infection in Taiwan: antibiotic resistance, serogroup distribution, and ribotype analysis. Microb Drug Resist. 2002;8:201–8. DOIPubMedGoogle Scholar
- Hsueh PR, Liu YC, Yang D, Yan JJ, Wu TL, Huang WK, Multicenter surveillance of antimicrobial resistance of major bacterial pathogens in intensive care units in 2000 in Taiwan. Microb Drug Resist. 2001;7:373–82. DOIPubMedGoogle Scholar
- Ho M, McDonald LC, Lauderdale TL, Yeh LL, Chen PC, Shiau YR. Surveillance of antibiotic resistance in Taiwan, 1998. J Microbiol Immunol Infect. 1999;32:239–49.PubMedGoogle Scholar
- Hsueh PR, Liu CY, Luh KT. Current status of antimicrobial resistance in Taiwan. Emerg Infect Dis. 2002;8:132–7.PubMedGoogle Scholar
- Su SC, Huang FY, Liu CP. Prevalence of penicillin-resistant Streptococcus pneumoniae at a medical center in Taipei. J Infect Dis Soc ROC. 1996;7:99–105.
- Hsueh PR, Wu JJ, Hsiue TR. Invasive Streptococcus pneumoniae infection associated with rapidly fatal outcome in Taiwan. J Formos Med Assoc. 1996;95:364–71.PubMedGoogle Scholar
- Wu TT, Hsueh PR, Lee LN, Yang PC, Luh KT. Pneumonia caused by penicillin-nonsusceptible Streptococcus pneumoniae: clinical characteristics, prognostic factors, and outcomes. J Formos Med Assoc. 2000;99:18–23.PubMedGoogle Scholar
- Huang FY, Chiu NC, Liu SC. Penicillin-resistant pneumococcal infections in children. J Formos Med Assoc. 1997;96:414–8.PubMedGoogle Scholar
- Lu CY, Lee PI, Hsueh PR, Chang SC, Chiu TF, Lin HC, Penicillin-nonsusceptible Streptococcus pneumoniae infections in children. J Microbiol Immunol Infect. 1999;32:179–86.PubMedGoogle Scholar
- Ma JS, Chen PY, Chi CS, Lin JF, Lau YJ. Invasive Streptococcus pneumoniae infections of children in central Taiwan. J Microbiol Immunol Infect. 2000;33:169–75.PubMedGoogle Scholar
- Chiang CJ, Hwang KP, Peng CF, Kuo CS. Antimicrobial resistance and serotype distribution of Streptococcus pneumoniae infections in Kaohsiung from 1996 through 1999. J Microbiol Immunol Infect. 2001;34:269–74.PubMedGoogle Scholar
- Fang CT, Hung CC, Chang SC, Hsueh PR, Chang YL, Chen MY, Pulmonary infection in human immunodeficiency virus-infected patients in Taiwan. J Formos Med Assoc. 2000;99:123–7.PubMedGoogle Scholar
- Wang CH, Lin TY. Invasive Haemophilus influenzae disease and purulent meningitis in Taiwan. J Formos Med Assoc. 1996;95:599–604.PubMedGoogle Scholar
- Liu CC, Chen JS, Lin CH, Chen YJ, Huang CC. Bacterial meningitis in infants and children in southern Taiwan: emphasis on Haemophilus influenzae type b infection. J Formos Med Assoc. 1993;92:884–8.PubMedGoogle Scholar
- Chang YC, Huang CC, Wang ST, Liu CC, Tsai JJ. Risk factors analysis for early fatality in children with acute bacterial meningitis. Pediatr Neurol. 1998;18:213–7. DOIPubMedGoogle Scholar
- Fang CT, Chang SC, Hsueh PR, Chen YC, Sau WY, Luh KT. Microbiologic features of adult community-acquired meningitis in Taiwan. J Formos Med Assoc. 2000;99:300–4.PubMedGoogle Scholar
- Li WC, Chiu NC, Hsu CH, Lee KS, Hwang HK, Huang FY. Pathogens in the middle ear effusion of children with persistent otitis media: implications of drug resistance and complications. J Microbiol Immunol Infect. 2001;34:190–4.PubMedGoogle Scholar
- Hsiao KM, Ni SL, Won AM, Lin TY. Penicillin, erythromycin, or chloramphenicol-resistant pneumococcus. Clin Pediatr J. 1986;27:345–51.
- Hsueh PR, Teng LJ, Lee LN, Yang PC, Ho SW, Lue HC, Increased prevalence of erythromycin resistance in streptococci: substantial upsurge in erythromycin-resistant M-phenotype in Streptococcus pyogenes (1979–1998) but not in Streptococcus pneumoniae (1985–1999) in Taiwan. Microb Drug Resist. 2002;8:27–33. DOIPubMedGoogle Scholar
- Hsueh PR, Teng LJ, Wu TL, Ho SW, Luh KT. First clinical isolate of Streptococcus pneumoniae exhibiting high-level resistance to fluoroquinolones in Taiwan. J Antimicrob Chemother. 2001;48:316–7. DOIPubMedGoogle Scholar
- Luh KT, Hsueh PR, Teng LJ, Pan HJ, Chen YC, Lu JJ, Quinupristin-dalfopristin resistance among gram-positive bacteria in Taiwan. Antimicrob Agents Chemother. 2000;44:3374–80. DOIPubMedGoogle Scholar
- Shi ZY, Enright MC, Wilkinson P, Griffiths D, Spratt BG. Identification of three major clones of multiply antibiotic-resistant Streptococcus pneumoniae in Taiwanese hospitals by multilocus sequence typing. J Clin Microbiol. 1998;36:3514–9.PubMedGoogle Scholar
- Hsueh PR, Teng LJ, Lee LN, Yang PC, Ho SW, Luh KT. Dissemination of high-level penicillin-, extended-spectrum cephalosporin-, and erythromycin-resistant Streptococcus pneumoniae clones in Taiwan. J Clin Microbiol. 1999;37:221–4.PubMedGoogle Scholar
- Liu PY, Hu BS, Fung CP, Lau YJ, Shi ZY, Lin YH. Molecular epidemiology of penicillin-resistant Streptococcus pneumoniae isolated in central Taiwan. Diagn Microbiol Infect Dis. 1998;31:511–5. DOIPubMedGoogle Scholar
- Huang YC, Wong KS, Hsueh PR, Lin TY. Bacteremic pneumonia caused by penicillin-resistant Streptococcus pneumoniae in siblings. Pediatr Infect Dis J. 1999;18:734–5. DOIPubMedGoogle Scholar
- Chiou CC, McEllistrem MC. Novel penicillin-, cephalosporin-, and macrolide-resistant clones of Streptococcus pneumoniae serotypes 23F and 19F in Taiwan which differ from international epidemic clones. J Clin Microbiol. 2001;39:1144–7. DOIPubMedGoogle Scholar
- Richter SS, Heilmann KP, Coffman SL, Huynh HK, Brueggemann AB, Pfaller MA, The molecular epidemiology of penicillin-resistant Streptococcus pneumoniae in the United States, 1994–2000. Clin Infect Dis. 2002;34:330–9. DOIPubMedGoogle Scholar
- Ip M, Lyon DJ, Yung RWH, Tsang L, Cheng AFB. Introduction of new clones of penicillin-nonsusceptible Streptococcus pneumoniae in Hong Kong. J Clin Microbiol. 2002;40:1522–5. DOIPubMedGoogle Scholar
- Ho PL, Yam WC, Cheung TK, Ng WW, Que TL, Tsang DN, Fluoroquinolone resistance among Streptococcus pneumoniae in Hong Kong linked to the Spanish 23F clone. Emerg Infect Dis. 2001;7:906–8.PubMedGoogle Scholar
- Quale J, Landman D, Ravishankar J, Flores C, Bratu S. Streptococcus pneumoniae, Brooklyn, New York: fluoroquinolone resistance at our doorstep. Emerg Infect Dis. 2002;8:594–7.PubMedGoogle Scholar
- Infectious Diseases Society of the Republic of China. Guidelines for antimicrobial therapy of pneumonia in Taiwan. J Microbiol Immunol Infect. 1999;32:292–4.PubMedGoogle Scholar
- Heffelfinger JD, Dowell SF, Jorgensen JH, Klugman KP, Mabry LR, Musher DM, Management of community-acquired pneumonia in the era of pneumococcal resistance: a report from the Drug-Resistant Streptococcus pneumoniae Therapeutic Working Group. Arch Intern Med. 2000;160:1399–408. DOIPubMedGoogle Scholar
- American Thoracic Society. Guidelines for the management of adults with community-acquired pneumonia: diagnosis, assessment of severity, antimicrobial therapy, and prevention. Am J Respir Crit Care Med. 2001;163:1730–54.PubMedGoogle Scholar
- Bartlett JG, Dowell SF, Mandell LA, File TM Jr, Musher DM, Fine AM. Practice guidelines for the management of community-acquired pneumonia in adults. Clin Infect Dis. 2000;31:347–82. DOIPubMedGoogle Scholar
- Chung ST, Lee JC, Shieh WC. Type distribution of pneumococcal strains in Taiwan. Chin J Microbiol Immunol. 1991;24:196–20.
- Chang SC, Shiu MN, Chen TJ. Antibiotic usage in primary care units in Taiwan after the institution of National Health Insurance. Diagn Microbiol Infect Dis. 2001;40:137–43. DOIPubMedGoogle Scholar
- Liu YC, Huang WK, Huang TS, Kunin CM. Extent of antibiotic use in Taiwan shown by antimicrobial activity in urine. Lancet. 1999;354:1360. DOIPubMedGoogle Scholar
Figures
Table
Cite This ArticleTable of Contents – Volume 8, Number 12—December 2002
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Po-Ren Hsueh, Department of Laboratory Medicine, National Taiwan University Hospital, No 7, Chung-Shan South Road, Taipei, Taiwan; fax: 886-2-23224263;
Top