Volume 13, Number 9—September 2007
Letter
Imported Fatal Hantavirus Pulmonary Syndrome
To the Editor: Hantavirus pulmonary syndrome (HPS) is characterized by fever, gastrointestinal symptoms, respiratory distress, elevated hematocrit, hypoalbuminemia, and thrombocytopenia. Most cases in North America are acquired from rodent vectors and are caused by the Sin Nombre virus. Person-to-person transmission has been reported for Andes virus (1,2) but not for Sin Nombre virus (3). We describe a patient with fatal hantavirus pulmonary syndrome.
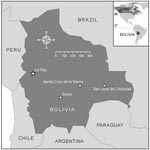
The patient was a previously healthy 15-year-old Canadian girl. In the spring of 2006, she had traveled to the Santa Cruz-San Jose de Chiquitas corridor of Bolivia with her parents and siblings for a 4-week visit (Figure), where they stayed with family and friends on their farms. The family noted rodent droppings outside but no rodents were seen. The patient had no known exposure to rodents or rodent droppings after her return to Canada.
On day 26 after her return from Bolivia, the patient sought treatment at a community hospital at 6:30
Serologic examination of an acute blood sample was immunoglobulin M (IgM) positive for Sin Nombre virus, but low optical densities indicated potential for an infection with a related hantavirus rather than Sin Nombre virus. Subsequently, reverse transcription–PCR (RT-PCR) on blood in EDTA and lung tissue followed by sequence analysis confirmed an Andes-like hantavirus infection. None of the 40 household and healthcare contacts of the patient had symptoms compatible with HPS during an 8-week monitoring period. Two contacts with nonspecific symptoms were tested and found to be negative for hantavirus-specific immunoglobulin (Ig) M and IgG and negative by RT-PCR.
Additonally, a seroprevalence survey of close contacts and assessment of level of contact was conducted. Close contacts were defined as persons who lived in the same household as the patient, were in the same enclosed space for >2 hours, or provided healthcare to her while she was symptomatic. Twenty-eight (62%) of 45 close contacts provided serum over the next 5 months. All serum samples were negative for Sin Nombre and Andes IgG and Sin Nombre IgM by ELISA. Fourteen (50%) of the 28 completed a self-administered questionnaire which assessed the type and intensity of contact. Of these, 12 were healthcare workers and 2 were friends. One friend had contact with the patient 3 days before she died, a friend and a healthcare worker had contact with her on the day before her death, and the rest of the healthcare workers had contact with the patient on the day she died.
To our knowledge, this is the first imported case and the tenth case of HPS reported in British Columbia, Canada, since 1994 (2005 BC Annual Summary of Reportable Diseases at www.bccdc.org/content.php?item=33) (4). Six of these 10 cases were fatal. All cases except the 1 described here have been locally acquired Sin Nombre infections. Sin Nombre virus is endemic in the Peromyscus maniculatus (deer mice) population in most of British Columbia (5).
Worldwide, imported cases of HPS are unusual, although HPS has been reported in countries that are in close geographic proximity or in travelers to disease-endemic areas (6–8). Fortunately, none of the persons exposed to the patient reported symptoms consistent with HPS during the incubation period, and none who were tested seroconverted. Seroprevalence surveys in Chile among healthcare worker contacts of patients with HPS caused by the Andes virus showed a prevalence of 0% (9). A report from Argentina showed that cases due to secondary transmission occurred mostly in non-healthcare workers after prolonged close contact in the prodromal period (10). In conclusion, we describe an imported case of fatal HPS due to an Andes-like hantavirus with no evidence of secondary transmission.
Acknowledgment
We thank Heinz Feldman and Harvey Artsob for coordinating the virologic workup and providing feedback on manuscript drafts; Deborrah McFadden for completing the autopsy; Bonnie Anderson for coordinating the local serosurveys; Sunny Mak for making the map used in the publication; and the public health staff at Northern Health Authority for conducting active surveillance and helping to coordinate the serosurvey.
References
- Wells RM, Sosa Estani S, Yadon ZE, Enria D, Padula P, Pini N, An unusual hantavirus outbreak in southern Argentina: person-to-person transmission? Hantavirus Pulmonary Syndrome Study Group for Patagonia. Emerg Infect Dis. 1997;3:171–4. DOIPubMedGoogle Scholar
- Wells RM, Young J, Williams RJ, Armstrong LR, Busico K, Khan AS, Hantavirus transmission in the United States. Emerg Infect Dis. 1997;3:361–5. DOIPubMedGoogle Scholar
- Vitek CR, Breiman RF, Ksiazek TG, Rollin PE, McLaughlin JC, Umland ET, Evidence against person-to-person transmission of hantavirus to health care workers. Clin Infect Dis. 1996;22:824–6.PubMedGoogle Scholar
- MacDougall L, Fyfe M, Bowie WR, Cooper K, McCauley GD, Morshed M. Hantavirus infection in British Columbia: an atypical case history and epidemiological review. BCMJ. 2005;47:234–40.
- Drebot MA, Artsob H, Werker D. Hantavirus pulmonary syndrome in Canada, 1989–1999. Can Commun Dis Rep. 2000;26:65–9.PubMedGoogle Scholar
- Espinoza R, Vial P, Noriega LM, Johnson A, Nichol ST, Rollin PE, Hantavirus pulmonary syndrome in a Chilean patient with recent travel in Bolivia. Emerg Infect Dis. 1998;4:93–5. DOIPubMedGoogle Scholar
- Castillo C, Nicklas C, Mardones J, Ossa G. Andes hantavirus as possible cause of disease in travellers to South America. Travel Med Infect Dis. 2007;5:30–4. DOIPubMedGoogle Scholar
- Murgue B, Domart Y, Coudrier D, Rollin PE, Darchis JP, Merrien D, First reported case of imported hantavirus pulmonary syndrome in Europe. Emerg Infect Dis. 2002;8:106–7. DOIPubMedGoogle Scholar
- Castillo C, Villagra E, Sanhueza L, Ferres M, Mardones J, Mertz GJ. Prevalence of antibodies to hantavirus among family and health care worker contacts of persons with hantavirus cardiopulmonary syndrome: Lack of evidence for nosocomial transmission of Andes virus to health care workers in Chile. Am J Trop Med Hyg. 2004;70:302–4.PubMedGoogle Scholar
- Martinez VP, Bellomo C, San Juan J, Pinna D, Forlenza R, Elder M, Person-to-person transmission of Andes virus. Emerg Infect Dis. 2005;11:1848–53.PubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 13, Number 9—September 2007
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Steven Reynolds, Critical Care Medicine, Vancouver Acute ICU2, JPPN 2nd Floor, Room 2438, 855 W 12th Ave, Vancouver, BC V5Z 1M9, Canada;
Top