Volume 14, Number 11—November 2008
Dispatch
Pyemotes ventricosus Dermatitis, Southeastern France
Abstract
We investigated 42 patients who had unusual pruritic dermatitis associated with a specific clinical sign (comet sign) in 23 houses in southeastern France from May through September 2007. Pyemotes ventricosus, a parasite of the furniture beetle Anobium punctatum, was the cause of this condition.
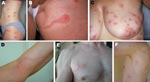
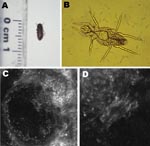
In 2006, we described an outbreak of unusual dermatitis in southeastern France (1). Patients affected had highly erythematous pruritic macules typical of arthropod bites, sometimes associated with a linear erythematous macular tract that we called the comet sign (Figure 1). The cause of this outbreak remained unknown. In May 2007, during an entomologic ecoenvironmental investigation conducted inside the homes of some of these patients, we found wooden furniture, which harbored live furniture beetles (Anobium punctatum) (Figure 2, panel A), and small amounts of wood dust on the floor. Because A. punctatum does not bite humans or cause contact dermatitis (2), it was not considered as the direct causative agent. However, stereomicroscope examination of the wood dust identified the mite Pyemotes ventricosus (Figure 2, panel B). Because Pyemotes spp. can cause dermatitis (3), they were considered as the hypothetical agent causing the eruption. We then conducted an observational and entomologic study of the new cases.
From May through September 2007, all patients referred to the dermatology department at Fréjus Hospital (Fréjus, France) with suspected arthropod-bite dermatitis were examined; patients were also checked for the comet sign. Patients were asked about their outdoor activities (walking in the countryside, gardening), homes, and whether they had wooden furniture potentially infested with furniture beetles. Skin eruptions were photographed. Detailed clinical and histologic descriptions of the lesions have been reported (1).
Whenever possible, ecoenvironments (surrounding terrain and home interior) of patients with typical macules associated with the comet sign were investigated. Household pets were examined by veterinarians. When wormholes were found in wooden furniture, A. punctatum was noted as present in the immediate environment. Mites were collected and examined under a stereomicroscope (magnification ×80). Removal of furniture was recommended if it was infested with A. punctatum.
From May through October 2007, 42 patients with typical eruption formed 23 clusters, comprising 1–5 patients each living in the same home. Nineteen patients lived <50 km from Fréjus and 23 were vacationing in this city. Among the 23 homes in the cluster, 14 were entomologically and ecoenvironmentally investigated. A. punctatum (Figure 2, panel A) was found in all 14 homes and P. ventricosus was found in 12 (83%). Females (Figure 2, panel B), some gravid, and rare males were seen. Entomologic investigations outside homes found no evidence of any other insect pests. Veterinarians who examined the 2 pets living in these homes excluded dog ectoparasites. Dermatitis persisted or recurred for weeks in all patients until infested furniture was removed or patients left their homes. Oral prednisone (0.5 mg/kg) rapidly (within 48 hours) attenuated the pruritus.
One of us (P.D.) volunteered to place P. ventricosus–infested wood dust on 1 cm2 of abdominal skin under an occlusive bandage for 4 hours. Two negative controls consisted of placing uncontaminated wood dust under a bandage and the bandage alone. Twenty-four hours later, an erythematous macular pruritic lesion was observed that lasted for 7 days, but no comet sign developed. No cutaneous reaction was observed under the 2 negative-control bandages.
Natural dermatitis also occurred in 2 investigators during collection of ecoenvironmental samples. Typical lesions with the comet sign (Figure 1, panels E and F) developed in these investigators after they touched wood dust and infested furniture (1 of the investigators had only entered a room with infested furniture but had not touched it). Skin scrapings of the investigators did not contain parasites. A skin-biopsy specimen from 1 investigator showed a subcorneal ulceration but no parasite. Skin lesions were examined dermoscopically (magnification ×40) and showed a microulceration or vesicle in the center of the macule. In contrast, in vivo confocal laser scanning microscopy (CLSM) of a microvesicle from 1 investigator showed an ovoid foreign body with morphologic features suggestive of P. ventricosus (Figure 2, panels C and D).
In 2006, we described an outbreak of an unusual dermatitis associated with a specific clinical sign that we called the comet sign (1). In 2007, similar cases occurred and we demonstrated that the mite P. ventricosus was the causative agent of the condition. P. ventricosus (Newport, 1850) (phylum Arthropoda, class Arachnida, order Acarina, suborder Prostigmata, family Pyemotidae) is an ectoparasite of arthropod larvae. This mite has been reported to be associated with A. punctatum (De Geer, 1774), the common furniture beetle (2).
This mite was associated with 2 investigators’ macular lesions that were acquired during experimental or natural infection. Natural infestation gave rise to macules frequently associated with the comet sign. We visualized, by using in vivo CLSM, a microvesicle, an ovoid foreign body with morphologic features suggestive of the mite. An entomologic ecoenvironmental investigation found P. ventricosus and its host (A. punctatum) in 83% of the patients’ homes investigated. Although Pyemotes spp.–related dermatitis outbreaks have been described, the outbreak we describe showed an emergent pattern with documented intradomiciliary infestation and the comet sign.
Although Pyemotes spp. have been known since the beginning of the 20th century to cause dermatitis (5), recent reports are scarce. In all recorded outbreaks, ectoparasites of insect larvae feeding on plants were responsible for dermatitis in workers exposed to agricultural products (3–7). Recent reports of dermatitis caused by Pyemotes spp. are even rarer (14 clinical reports since 1961), which make this dermatitis an almost forgotten disease (8–13).
The outbreak was associated with home interior infestations of P. ventricosus associated with A. punctatum. Fine and Scott described the first cases of dermatitis caused by P. ventricosus parasitizing A. punctatum (8). In Great Britain, Hickin found that up to 60% of woodworm larvae in damp locations were parasitized with Pyemotes spp., which were considered responsible for some skin irritations in woodsmen (2). More recently, Rodriguez-Casado et al. (11) described a P. dermatitis outbreak associated with A. punctatum–infested wood desks in a school.
Our cases were concentrated from May through September. The fact that we observed most cases in July and August might reflect the mite’s life cycle, which is activated when temperatures reach 80°F (26°C) (3). Moreover, many patients (23/42 in 2007) were on summer vacation, and most of them were living in homes that had been closed for months (i.e., not cleaned regularly), making it likely that the interior mite concentration would be high.
Pyemotes spp. dermatitis has been described as a pruritic erythematous rash with maculopapules with a central microvesicle (7). We initially reported that the typical pruritic erythematous macules were sometimes associated with a linear tract (comet sign) (1). Several hours after exposure, a linear erythematous macular tract arose from patients’ lesions. Whether this sign is specific to Pyemotes spp. or P. ventricosus remains unknown. The epidermis along the linear tract was clinically and histologically intact (1), thereby making contact dermatitis or epidermal migration of P. ventricosus, as in human scabies, unlikely. In vivo CLSM detected features suggestive of the mite inside the cutaneous microvesicle. A comet sign might represent onset of specific lymphangitis, as suggested for 1 patient (Figure 1, panel D). Two recent similar cases in southern France, which were considered specific atypical lymphangitis (14,15), might have been P. ventricosus dermatitis.
Dr Del Giudice is head of the infectious diseases and dermatology unit at Hôpital Bonnet, Fréjus, France. He researches skin infections.
Acknowledgments
We thank Geneviève Guérard for referring patients, Jean François Michiels and Yves le Fichoux for helpful comments, and Janet Jacobson for reviewing the English.
The confocal scanning laser microscope used in this study was obtained through a grant from the Conseil General des Alpes-Maritimes.
References
- Del Giudice P, Caumes E, Boissy C, Leduff F, Delaunay P, Blanc-Amrane V, An outbreak of creeping eruption in southern France. Br J Dermatol. 2007;157:824–5. DOIPubMedGoogle Scholar
- Hickin E. The woodworm. Science Journal. 1969;3:64–70.
- Hewitt M, Barrow GI, Miller DC, Turk SM. A case of Pyemotes dermatitis, with a note on the role of these mites in skin disease. Br J Dermatol. 1976;94:423–30. DOIPubMedGoogle Scholar
- Cross EA, Moser JC. A new dimorphic species of Pyemotes and key to previously described forms (Acarina: Tarsonemoidea). Ann Entomol Soc Am. 1975;68:723–32.
- Letchford J, Strungs I, Farrell D. Pyemotes species strongly implicated in an outbreak of dermatitis in a Queensland country hospital. Pathology. 1994;26:330–2. DOIPubMedGoogle Scholar
- Swan DC. The hay itch mite Pediculoides ventricosus (Newport) (Acarina, Pediculoidae) in South Australia. Journal of Agricultural India and South Australia. 1934;37:1289–99.
- Booth BH, Jones RWBB. Epidemiological and clinical study of grain itch. JAMA. 1952;150:1575–9.
- Fine RM, Scott HG. Straw itch mite dermatitis caused by Pyemotes ventricosus: comparative aspects. South Med J. 1965;58:416–20.PubMedGoogle Scholar
- Rycroft RJ, Kennedy C. Pyemotes dermatitis in display artists. Clin Exp Dermatol. 1981;6:629–34. DOIPubMedGoogle Scholar
- Betz TG, Davis BL, Fournier PV, Rawlings JA, Elliot LB, Baggett DA. Occupational dermatitis associated with straw itch mites (Pyemotes ventricosus). JAMA. 1982;247:2821–3. DOIPubMedGoogle Scholar
- Rodríguez-Casado MJ, Cerro-González R, Martín-Blázquez JL, Vázquez-Contioso M. Outbreak of Pyemotes dermatitis in an elementary school [in Spanish]. Enferm Infecc Microbiol Clin. 2004;22:370–1. DOIPubMedGoogle Scholar
- Broce AB, Zurek L, Kalish JA, Brown R, Keith DL, Gordon D, Pyemotes herfsi (Acari: Pyemotidae), a mite new to North America as the cause of bite outbreaks. J Med Entomol. 2006;43:610–3. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Outbreak of pruritic rashes associated with mites—Kansas, 2004. MMWR Morb Mortal Wkly Rep. 2005;54:952–5.PubMedGoogle Scholar
- Abraham S, Tschanz C, Krischer J, Saurat JH. Lymphangitis due to insect sting. Dermatology. 2007;215:260–1. DOIPubMedGoogle Scholar
- Marque M, Girard C, Guillot B, Bessis D. Dermite érythémateuse linéaire supra-lymphatique réactionnelle: une nouvelle entité clinico-histologique (poster no. 121). In: Abstracts of the Paris Dermatology Meeting. 5–9 December 2006, Paris, France. Ann Dermatol Venereol. 2006;133:4S1–298.
Figures
Cite This ArticleTable of Contents – Volume 14, Number 11—November 2008
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Pascal Del Giudice, Unité de Maladies Infectieuses et Dermatologie, Hôpital Bonnet, Ave André-Léotard, 83700 Fréjus, France;
Top